The most common are shortness of breath and lingering cough: Study
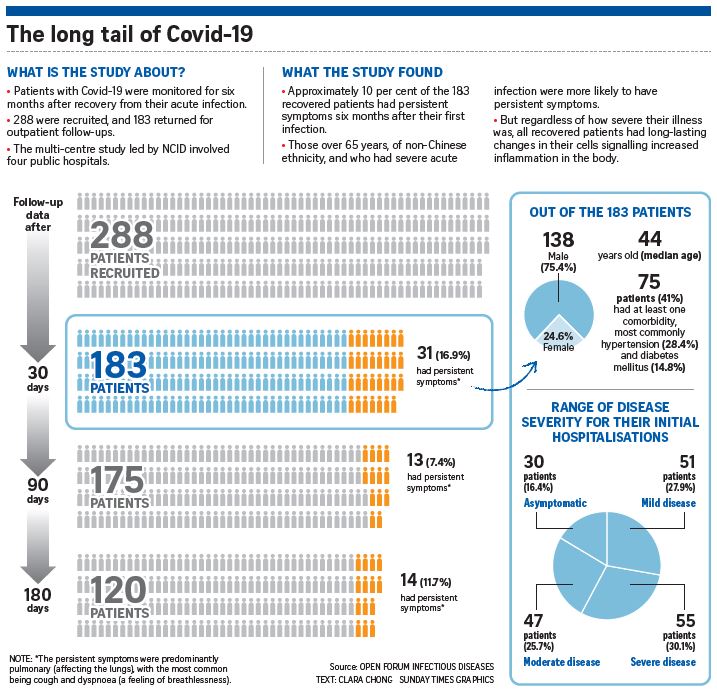
One in 10 recovered COVID-19 patients had persistent symptoms six months after the initial infection, a study led by the National Centre for Infectious Diseases (NCID) has found.
In this condition known as “long COVID”, the patients continued to experience symptoms, most commonly a lingering cough and shortness of breath, long after recovering from COVID-19. Other symptoms included persistent fatigue, dizziness and insomnia, but these were not frequently observed.
More importantly, the study also found elevated inflammatory markers regardless of whether the person had a serious or mild case of the disease. These proteins in the blood have been associated with conditions affecting the circulatory system and are a risk factor for cardiovascular disease.
Long COVID is a serious concern that, if widespread, will likely put a strain on the society and economy for years to come, said experts The Sunday Times spoke to previously on the matter.
It adds to the hidden toll of the pandemic, with the long period of less-than-optimal health signalling the critical need for people to avoid infection in the first place.
The study led by NCID involved three other public hospitals. Patients typically joined the study during their first week of illness and were monitored for six months.
A total of 288 patients were recruited, and 183 of them returned for outpatient follow-ups.
People over 65 years old, of non-Chinese ethnicity, and who had severe illness were more likely to have persistent symptoms. The reason for the association with non-Chinese ethnicity is unclear.
The study began in mid-January last year soon after the first case was detected in Singapore, with the aim of studying the long-term impact of COVID-19, up to two years post-infection, and also to understand how any protective immunity from infection evolves over time.
Dr Barnaby Young, a consultant at NCID who was involved in the study, said: “We understand from cases who passed on... that although the lungs are the major organ affected, the virus actually caused wider damage.”
This included damage to the heart as well as the inner lining of small blood vessels.
In some individuals, the Sars-CoV-2 virus, which causes COVID-19, damages blood vessels, and in particular small vessels that are present in every part of the body, leading to blockage of the blood supply and bleeding.
Dr Young noted that much is still unknown about long COVID.
The symptoms can be wide-ranging and non-specific, and of varying duration, though the mechanisms that cause it are unclear.
International bodies like the World Health Organisation are also actively gathering more information.
The NCID is embarking on another study of whether there are long-term inflammatory consequences to COVID-19.
By taking blood from study subjects, the NCID aims to identify the mechanisms behind the inflammation and determine the groups at risk. Patients have been recruited steadily since April and preliminary results are expected in the next six months.
Dr Young also noted that though clear data is still lacking, it is likely that vaccination will help to prevent long COVID.
“This is because in those individuals who do get COVID-19 despite vaccination, the immune response induced by the vaccine is still able to significantly reduce the severity of the infection,” he said.
Recovered COVID-19 patient Sylvia Sim, 58, said that it took her about a year to regain her sense of smell completely. She tested positive for the virus on April 6 last year and was discharged on April 25.
“When I was first diagnosed, I was down with a fever and lost my sense of smell and taste. My sense of taste returned only some six months later and my sense of smell a year later. Till today, I am sometimes unable to smell,” she said.
Madam Sim’s condition would fit under long COVID, Dr Young said.
“Some aspects of long COVID relate more to a ‘post-viral syndrome’ with prolonged lethargy, dizziness and other symptoms. Loss of taste and smell may fit in as well,” he said.
Other complications such as blood clots may also be considered to be part of long COVID, he added.
“These different presentations are probably all related to each other but may be driven by different combinations of chronic inflammation, specific aspects of the immune response to infection or possibly residual viral fragments.”
Studies elsewhere are also showing the pandemic’s debilitating effects from long COVID. A study last month, tracking the health insurance records of nearly two million people in the United States who contracted the coronavirus last year, found that almost one-quarter of them sought medical treatment for new conditions, such as nerve and muscle pain, high cholesterol, high blood pressure and fatigue.
Read the full article here.
Source: The Straits Times © Singapore
Press Holdings Limited. Permission required for reproduction.